|
Higher 28-day mortality was associated with being older, being male, and having comorbidities. They determined that the Alpha, BA.2, and BA.5 variants were associated with lower 28-day mortality than Delta, findings that were confirmed with Cox proportional hazards model. The investigators performed a logistic regression analysis with patient 28-day hospital mortality as the dependent variable. 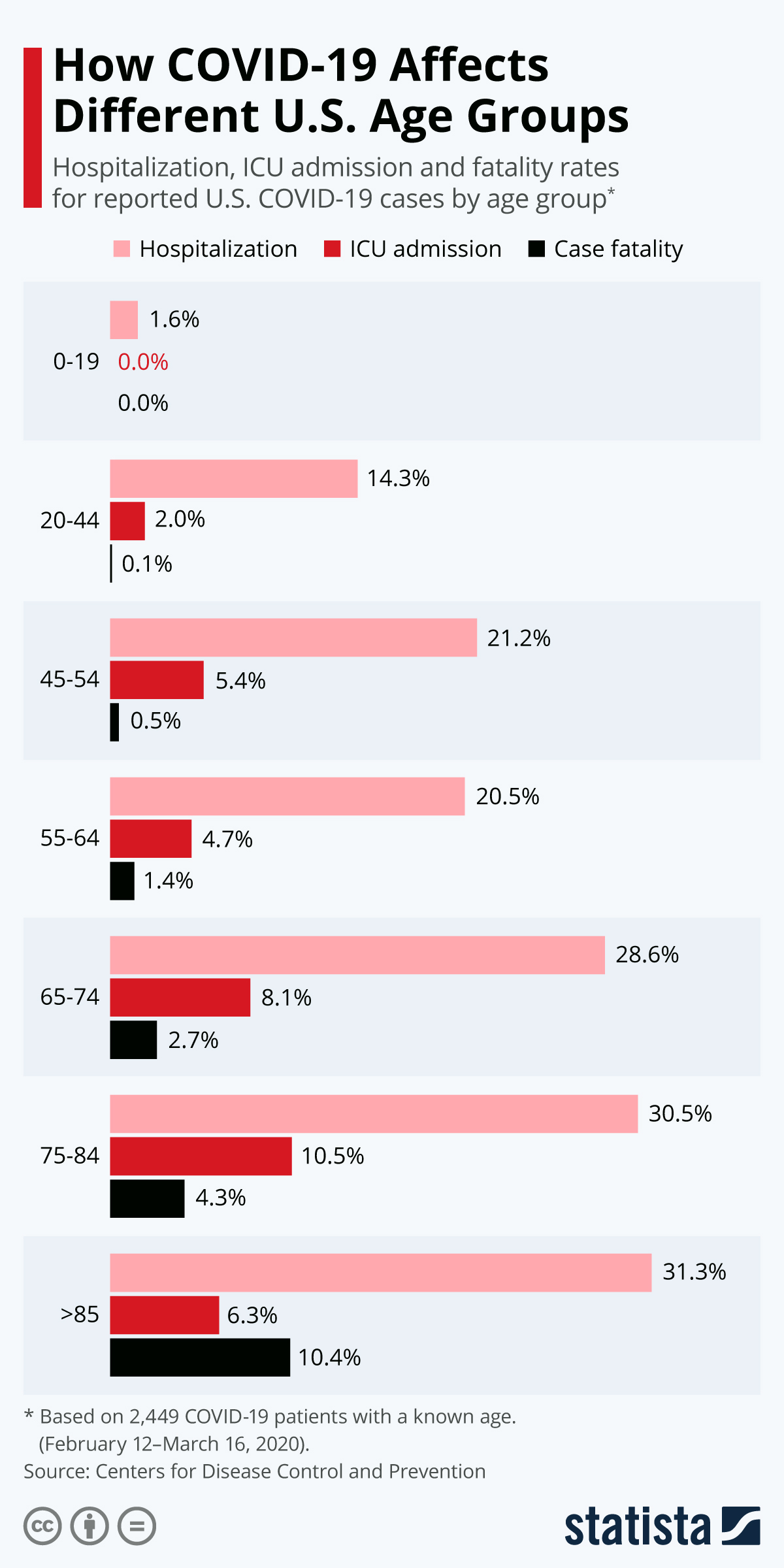
The median age of hospitalized Alpha patients was 57 years, Delta was 59 years, BA.1 was 73 years, BA.2 was 80 years, and BA.5 was 80.5 years. The investigators found there was a larger age distribution in the patients who contracted Alpha or Delta, compared to those infected with Omicron sublineages. These findings confirmed that the reinfection rate for BA.2 was significantly lower when primary infection was caused by another BA.2 sublineage, rather than by another lineage.Ī total of 1144 COVID-19 patients were hospitalized during the study period. For the Delta and BA.1, the number of reinfections was higher for lineages that emerged earlier in the pandemic than those than those that spread more closely to the lineage causing the reinfection. There were 4 reinfections within the same variant: 2 patients infected with different sublineages of Delta, and 2 with different sublineages of BA.1 and BA.2. Notably, the investigators did not find reinfections from any variants circulating before Delta. Throughout the December 19, 2020-Jstudy period, the BA.5 variant was associated with the highest number of reinfections more than 2% of BA.5 cases were reinfections. 
There was a total of 127 reinfections, 2 in patients who were each reinfected twice. 
A total of 2859 samples were assigned to Alpha (B.1.1.7 and sublineages), and 6637 samples were assigned to Delta (B.1.617.2 and sublineages). Of the sequenced 27363 samples, 21745 passed the quality control and were assigned to a COVID-19 variant lineage. To gauge association between the lineage causing the infection and 28-day hospital mortality, the investigators utilized logistic regressions and Cox proportional hazards models. The investigators determined whether there was a difference in reinfection rates by performing a pairwise proportions test with post hoc Holm correction or a Fisher’s exact test with post hoc Holm correction. Reinfections also included cases caused by different lineages in primary and secondary infections.ĭescriptive statistics were collected, including patient age, sex, comorbidities, length of hospitalization, intensive care unit (ICU admission), and mortality. They determined reinfections by individuals with 2 sequenced positive COVID-19 samples with a time distance of > 90 days. 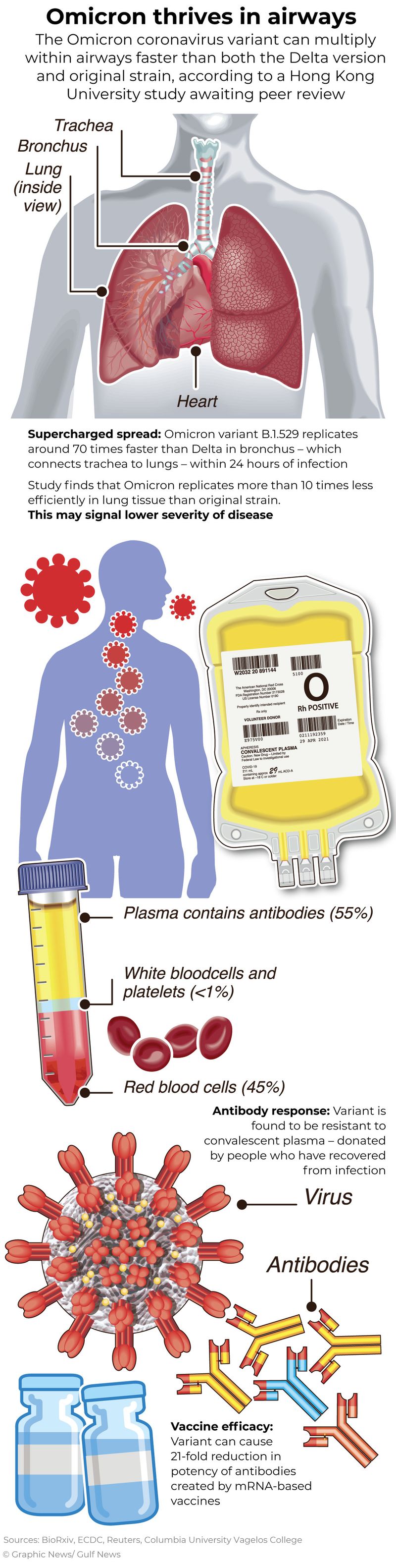
The investigators calculated reinfection rates, normalizing the number of reinfections caused by 1 lineage by the total number of samples assigned to that lineage in the dataset. The swabs underwent RT-qPCR testing to confirm COVID-19 seropositivity, and positive samples with a Ct ≤ 30 were sequenced. To truly assess the impact of Omicron, one study, presented this week at the 2023 European Congress of Clinical Microbiology & Infectious Diseases ( ECCMID), determined the reinfection rates and disease severity of Omicron sublineages and previous variants of concern (VOCs).įrom December 19, 2020-July 26, 2022, the investigators sequenced a total of 27363 nasopharyngeal swab samples from COVID-19 patients in the Canary Islands region of Spain. Omicron has long surpassed other COVID-19 lineages, with Omicron variants and subvariants responsible for nearly all COVID-19 infections worldwide.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
